Cystic Neoplasms
of the Pancreas
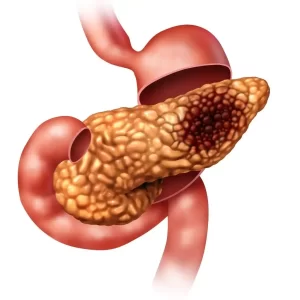
Cystic neoplasms are pre-malignant lesions that develop in the pancreas. They are more common in elderly individuals and usually discovered incidentally on imaging that is performed for other reasons. The cystic neoplasms of the pancreas are usually asymptomatic, but in some cases can cause jaundice, pancreatic insufficiency, or pancreatitis. Small cysts and cysts that have no worrisome features on imaging usually have a very low risk of developing into pancreatic cancer. Periodic imaging studies are performed to monitor these individuals over a number of years with small pancreatic cysts to ensure they are not growing rapidly. Cystic neoplasms that are larger than 3cm or have high-risk or worrisome features have a higher risk of harboring or developing into pancreatic cancer. The pancreatic doctor recommended surgery to remove the portion of the pancreas that contains the cystic neoplasm in this group of individuals who are fit for major abdominal surgery.
The work-up of cystic neoplasms of the pancreas can include imaging studies such as an MRI or CT scan to evaluate the size, location, and characteristics of the cyst. High-risk features include cystic lesions causing jaundice, cysts with large nodules on the cyst wall, and cystic lesions of the main duct with a large diameter.
Whipple procedure
This procedure involves removing the head of the pancreas, duodenum, and the distal bile duct followed by reconstruction. It is utilized for cystic neoplasms located in the head of the pancreas.
Distal Pancreatectomy
This procedure is for cystic neoplasms in the body or tail of the pancreas. Depending on the characteristics of the cyst, the spleen may be removed together with the distal pancreas to improve lymph node harvest.
Before surgery
The steps followed before surgery are:
- An office visit for surgical consultation where a comprehensive history and physical exam is performed.
- Completion of clinical tests for workup and staging.
- Multidisciplinary tumor board review for an expert recommendation regarding treatment strategy.
After surgery
The type of surgical procedure done determines the kind of post-surgery care required. Post care after a surgical operation involves:
- A brief admission to the ICU is sometimes required for complex procedures such as a whipple procedure. Recovery then continues in the hospital ward for another three to five days. Procedures performed robotically typically have a faster recovery and can expect discharge from the hospital one or two days earlier than after open procedures.
- The goals of postoperative care include: monitoring for and intervening on any complications that can occur, awaiting the resumption of normal bowel function, maintaining adequate hydration and nutrition, physical and occupational rehabilitation, and providing adequate pain control. Once these measures are met, the patient will be discharged from the hospital. Post-operative follow-up will be scheduled one week from discharge with Dr. Tierney.
