Dr. Joshua S. Tierney
Hepatopancreatobiliary (HPB) Surgery, Robotic Surgery, and Interventional Endoscopy/ERCP
Dr. Joshua Tierney is a published, award-winning, and fellowship-trained surgeon who treats patients from the Northern Front Range and Eastern Plains of Colorado, Wyoming, and Western Nebraska. He is board-certified in General Surgery and Fellowship-trained in Hepatopancreatobiliary (HPB) Surgery and ERCP.

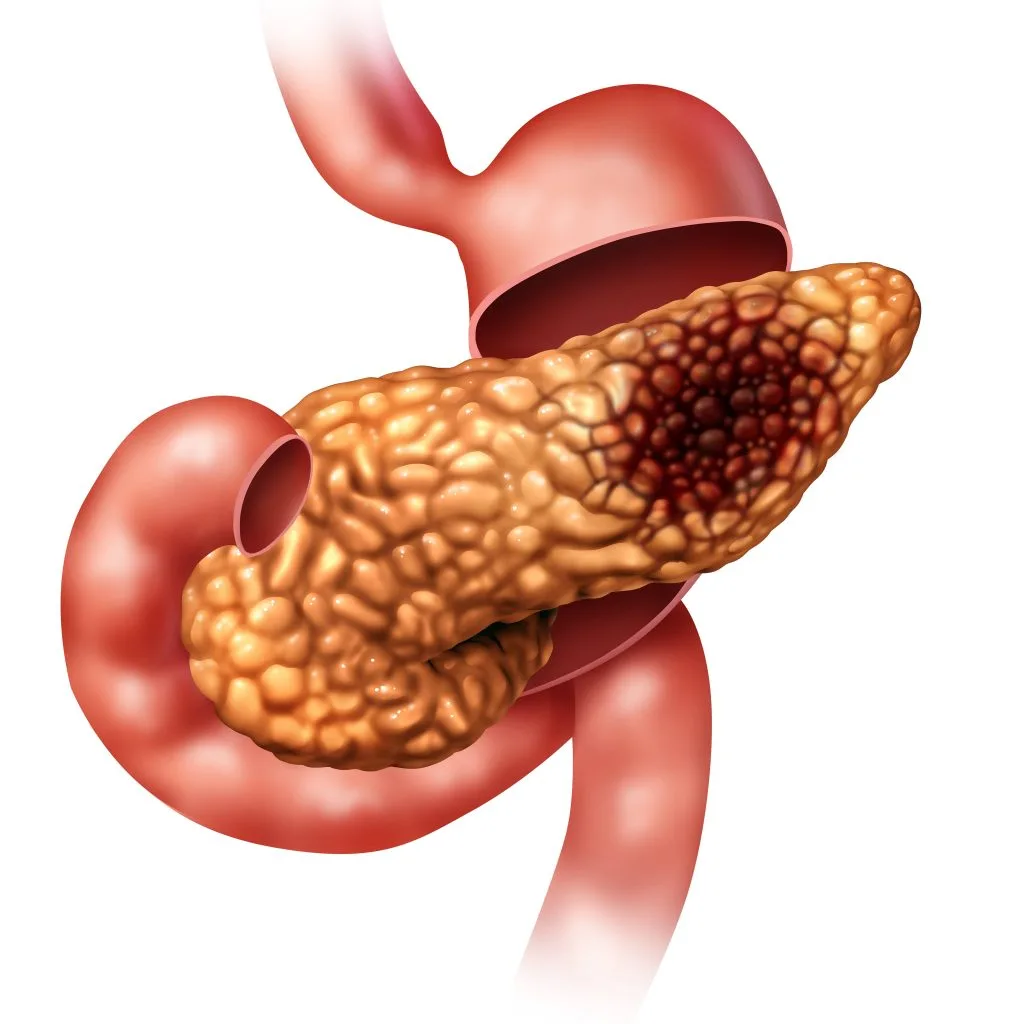
 How to diagnose pancreatic cancer early? Pancreatic cancer is usually diagnosed after a physician suspects the diagnosis and orders a CT scan to evaluate conditions of the pancreas or discovered incidentally on a CT scan obtained for other reasons. When a pancreatic mass is discovered on imaging a thorough workup is performed to establish the diagnosis, stage the disease, and determine if the tumor is resectable surgically. The additional tests employed include: blood tests, endoscopic ultrasound, endoscopic retrograde cholangiopancreatography (ERCP), and sometimes MRI or additional CT scan in hospital. After the workup is complete the case is discussed in a multidisciplinary tumor board where best pancreatic surgeon in Cheyenne, WY, discuss each case and determine the proper treatment strategy.
How to diagnose pancreatic cancer early? Pancreatic cancer is usually diagnosed after a physician suspects the diagnosis and orders a CT scan to evaluate conditions of the pancreas or discovered incidentally on a CT scan obtained for other reasons. When a pancreatic mass is discovered on imaging a thorough workup is performed to establish the diagnosis, stage the disease, and determine if the tumor is resectable surgically. The additional tests employed include: blood tests, endoscopic ultrasound, endoscopic retrograde cholangiopancreatography (ERCP), and sometimes MRI or additional CT scan in hospital. After the workup is complete the case is discussed in a multidisciplinary tumor board where best pancreatic surgeon in Cheyenne, WY, discuss each case and determine the proper treatment strategy.
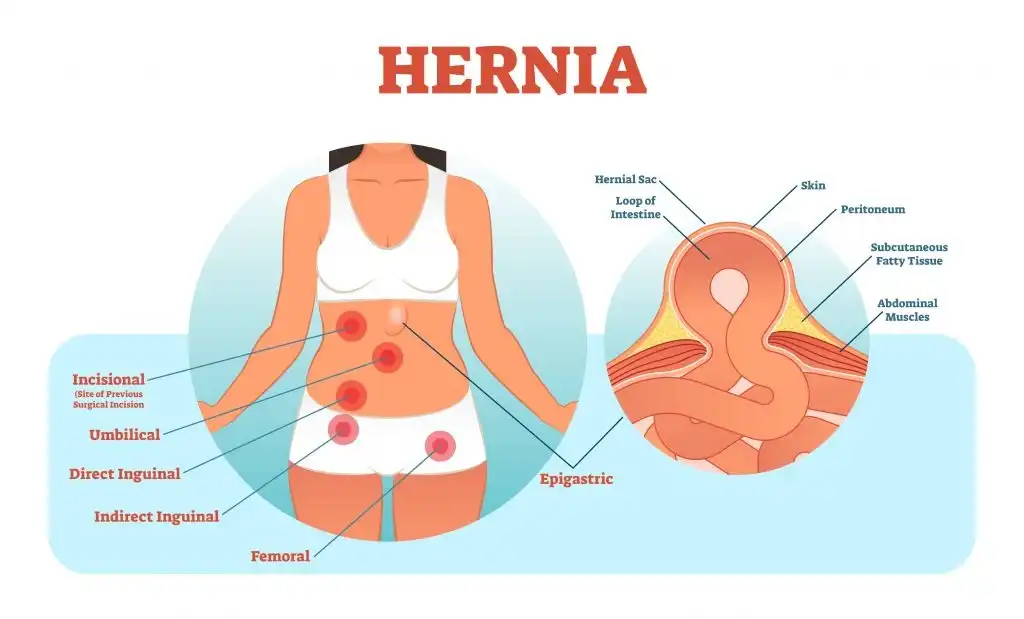 A hernia disease occurs when internal tissues or organs push through the wall holding them. The most common is an abdominal hernia where fatty tissue protrudes through a hole in the stomach wall, causing a bulge under the skin. Hernias are defects within the groin or abdominal walls that cause the abdomen’s contents to push out through these defects. Hernias are commonly situated at the groin and umbilicus because these areas in the abdominal wall feature congenital weakness. This may be caused by undue pressure e.g. heavy lifting, or weakness in the stomach wall e.g. from prior surgery. Hernias also form at the site of an incision from previous surgery. This type of hernia is also known as an incisional hernia. Hernias usually present as a protrusion or bulge that comes with a feeling of discomfort around the site, which may increase during physical exertion.
A hernia disease occurs when internal tissues or organs push through the wall holding them. The most common is an abdominal hernia where fatty tissue protrudes through a hole in the stomach wall, causing a bulge under the skin. Hernias are defects within the groin or abdominal walls that cause the abdomen’s contents to push out through these defects. Hernias are commonly situated at the groin and umbilicus because these areas in the abdominal wall feature congenital weakness. This may be caused by undue pressure e.g. heavy lifting, or weakness in the stomach wall e.g. from prior surgery. Hernias also form at the site of an incision from previous surgery. This type of hernia is also known as an incisional hernia. Hernias usually present as a protrusion or bulge that comes with a feeling of discomfort around the site, which may increase during physical exertion. Hernias are tears or holes in the abdominal or groin wall through which inner tissues protrude. A hernia causes pain and can lead to more complicated strangulation of the intestines. Hernia surgery is done to push back the protruding tissue and repair the hole. The weak point is reinforced with mesh.
Hernias are tears or holes in the abdominal or groin wall through which inner tissues protrude. A hernia causes pain and can lead to more complicated strangulation of the intestines. Hernia surgery is done to push back the protruding tissue and repair the hole. The weak point is reinforced with mesh. Robotic hernia surgery in Cheyenne, WY is a relatively new technique used to treat smaller hernias and rebuild the abdominal wall. Laparoscopic surgery requires a surgeon to hold the instruments, while robotic surgery features tools operated by a robot and controlled by the surgeon.
Robotic hernia surgery in Cheyenne, WY is a relatively new technique used to treat smaller hernias and rebuild the abdominal wall. Laparoscopic surgery requires a surgeon to hold the instruments, while robotic surgery features tools operated by a robot and controlled by the surgeon.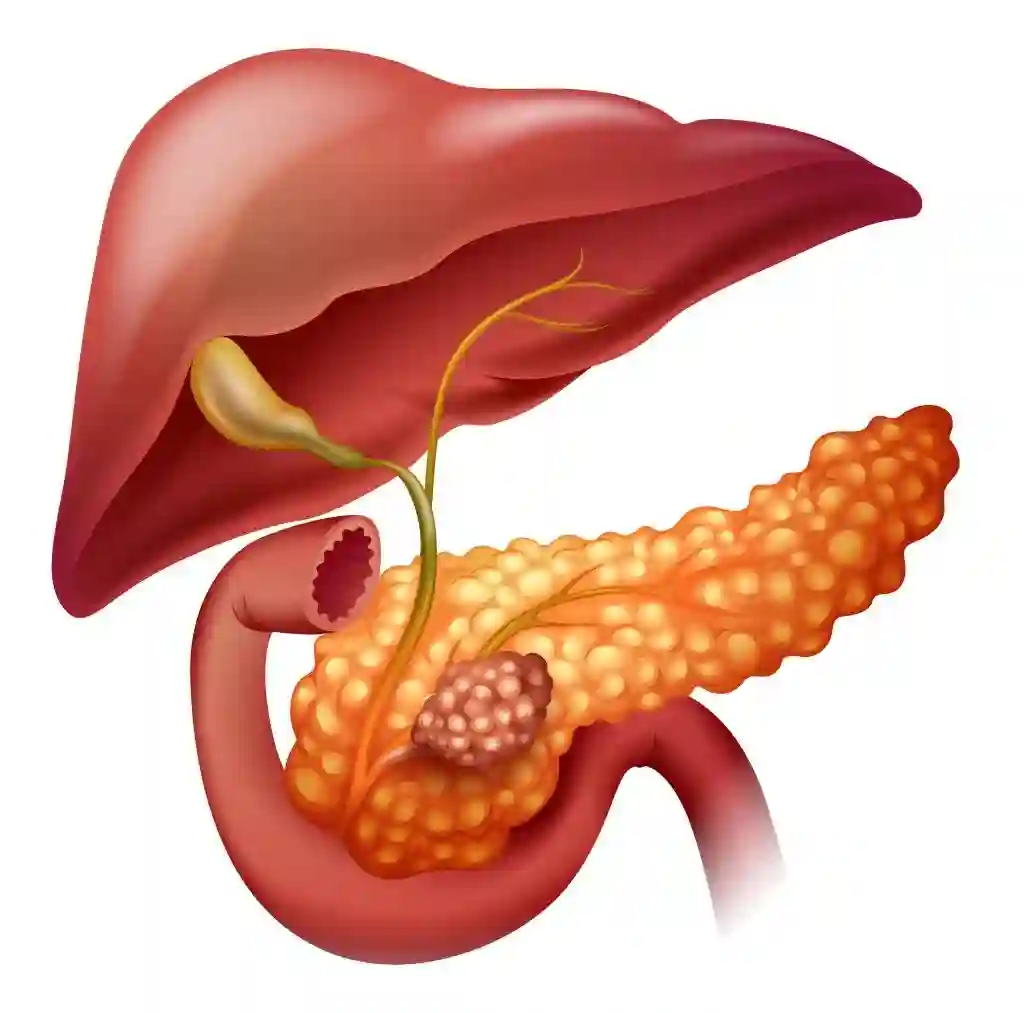 The Whipple procedure is a type of HPB Surgery & Oncology treatment that is recommended for advanced pancreatic cancer that has spread to the small intestines, gallbladder, and bile ducts. This procedure is also known as a pancreaticoduodenectomy. It involves removing the head of the pancreas, the duodenum, the distal bile duct, and the gallbladder. This procedure is performed when the tumor is located in the head of the pancreas. In the late stages of pancreatic cancer, the gallbladder, bile duct, and the first part of the small intestines become affected by the disease as well.
The Whipple procedure is a type of HPB Surgery & Oncology treatment that is recommended for advanced pancreatic cancer that has spread to the small intestines, gallbladder, and bile ducts. This procedure is also known as a pancreaticoduodenectomy. It involves removing the head of the pancreas, the duodenum, the distal bile duct, and the gallbladder. This procedure is performed when the tumor is located in the head of the pancreas. In the late stages of pancreatic cancer, the gallbladder, bile duct, and the first part of the small intestines become affected by the disease as well.